| Apr 14, 2026 |
Ferrocene-modified covalent organic frameworks combine sonodynamic therapy with immune activation to suppress primary breast tumors and bone metastasis in mice.
(Nanowerk News) A nanoscale therapeutic platform that pairs ultrasound-activated cancer treatment with immune system reprogramming has shown strong results against both primary breast tumors and bone metastasis in mice. The platform relies on ferrocene-modified covalent organic frameworks (mCOFs) that generate two types of reactive oxygen species to kill tumor cells while simultaneously provoking an antitumor immune response.
|
|
The study was published in Cyborg and Bionic Systems (“Ferrocene-Modified Nanoscale Covalent Organic Frameworks for Ferroptosis-Based Sonodynamic Therapy Inhibit Breast Cancer and Its Bone Metastasis”).
|
Key Findings
- Ferrocene-modified covalent organic frameworks combined with ultrasound reduced breast cancer cell viability to 24.3% and raised the apoptosis rate to 84.51% in laboratory tests.
- The treatment triggered robust immunogenic cell death, including a nearly fivefold increase in ATP release and a more than fourfold rise in dendritic cell maturation.
- In mouse models, the nanoplatform suppressed primary tumor growth, reduced metastatic bone destruction, and boosted antitumor immune cell infiltration.
|
|
Breast cancer is among the most prevalent cancers in women worldwide. Survival rates have improved over recent decades, but metastatic disease remains a stubborn clinical problem. Bone metastasis contributes heavily to poor outcomes and mortality, and most current therapies concentrate on controlling primary tumors with limited effectiveness at distant metastatic sites.
|
|
Sonodynamic therapy uses ultrasound to activate specialized sensitizer molecules inside tumors. The approach can penetrate deep into tissue and be controlled precisely in both space and time, making it attractive for treating solid tumors. But existing sonosensitizers have practical shortcomings. Inorganic versions resist biodegradation, while organic small-molecule sensitizers are difficult to equip with multiple therapeutic functions.
|
|
Covalent organic frameworks offer a potential way forward. These porous crystalline materials can be chemically tuned and show favorable biological compatibility, making them candidates for carrying multiple therapeutic payloads at once.
|
 |
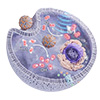
| Schematic showing the preparation of mCOFs and their role in tumor growth inhibition. TAPP, tetra (p-amino-phenyl) porphyrin; BPTA, 2,5-bis(2-propynyloxy) terephthalaldehyde; DHTA, 2,5-dihydroxyterephthalaldehyde; O-DCB, o-dichlorobenzene; BuOH, n-butanol; HMGB1, high mobility group box 1 protein; CRT, calreticulin; DC, dendritic cell. (Image: Ming Wu, Gongli Hospital of Pudong New Area)
|
|
“Sonodynamic therapy (SDT), with its deep tissue penetration and strong spatiotemporal controllability, has emerged as a promising approach for solid tumor treatment; however, currently available multifunctional sonosensitizers still face key limitations, including poor biodegradability in inorganic systems and limited multifunctionalization in organic small molecules,” said Ming Wu, a researcher at Gongli Hospital of Pudong New Area. “Against this backdrop, covalent organic frameworks (COFs), owing to their tunable structures, favorable biocompatibility, and functionalization potential, are increasingly regarded as promising platforms for next-generation multifunctional sonodynamic therapy.”
|
|
To build the mCOF platform, the team reacted microscale COFs with aminoferrocene using a top-down strategy. This step simultaneously shrank the particles to nanoscale dimensions and introduced iron-based catalytic sites. Under ultrasound exposure, the mCOFs generate singlet oxygen. The iron centers in ferrocene then convert hydrogen peroxide naturally present in the tumor microenvironment into hydroxyl radicals through Fenton-like chemistry, amplifying oxidative damage through a dual reactive oxygen species (ROS) mechanism.
|
|
The researchers characterized mCOFs for particle size, dispersibility, crystalline structure, and ROS-generation capacity, then tested their effects in 4T1 breast cancer cells. Combined with ultrasound, the mCOFs drove large increases in intracellular singlet oxygen and hydroxyl radical levels. Cell viability fell to 24.3%, and the apoptosis rate reached 84.51%. Strong lipid peroxidation confirmed that ferroptosis, a form of iron-dependent cell death driven by lipid damage, acted alongside apoptosis to produce the overall tumor-killing effect.
|
|
The treatment also activated immunogenic cell death, a process that alerts the immune system to tumor cells. ATP release climbed from 0.37 nM to 1.75 nM, and dendritic cell maturation rose from 5.27% to 23.6%. Levels of the pro-inflammatory cytokines IL-6 and TNF-α increased by 3.81-fold and 3.14-fold, respectively. These signals are essential for priming an adaptive antitumor immune response.
|
|
Animal experiments used orthotopic breast tumor and bone metastasis mouse models with intravenous mCOF administration. The nanoparticles accumulated efficiently at tumor sites within 12 hours of injection. Ultrasound activation at that point produced clear suppression of primary tumor growth. The treatment also reduced osteolytic bone destruction caused by metastatic cells, with measurements showing improved bone volume fraction and bone mineral density.
|
|
Immune profiling revealed broad activation across multiple cell types in treated animals. Mature dendritic cells, CD4+ and CD8+ T cells, natural killer cells, and IFN-γ-positive CD8+ T cells all showed increased infiltration into the tumor microenvironment. This pattern indicates that the platform reverses the immunosuppressive conditions tumors typically exploit to evade detection and spread.
|
|
“By introducing therapeutically active ferrocene moieties during the nanosizing of COFs, we provide a new design strategy for multifunctional sonosensitizers and further demonstrate the promising potential of nanomedicine-based combination therapies for suppressing breast cancer progression and bone metastasis,” said Ming Wu.
|
|
The dual-action approach demonstrated here, combining direct tumor cell destruction with immune remodeling, addresses a central limitation in current breast cancer treatment by extending therapeutic reach beyond the primary tumor site to metastatic bone lesions. The authors include Ming Wu, Yiqing Zeng, JianGang Chen, Zhen Yang, Siyuan Song, Rongkai Yan, Taofik Al Hassan, and Yan Zhang.
|