| Mar 11, 2026 |
A proof of principle study in mice shows mRNA-based polymer nanoparticles can reprogram T cells to eliminate B cells linked to lupus and blood cancers.
(Nanowerk News) Researchers at Johns Hopkins Medicine have engineered a simplified biodegradable nanoparticle that reprograms the immune system’s T cells to locate and destroy disease-causing B cells throughout the body. The polymer-based nanoparticles, tested in mice, eliminated 95% of targeted B cells in circulating blood within 24 hours of a single injection, offering a potential alternative to conventional CAR-T cell therapies for conditions such as lupus, leukemia, and lymphoma.
|
Key Findings
- A single dose of the nanoparticles depleted 95% of target B cells in the blood and roughly 50% in the spleen of healthy mice within 24 hours.
- The polymer-based nanoparticles require only three components, compared with the five components used in recently developed lipid-based alternatives.
- About 10% of the nanoparticles successfully escape cellular degradation compartments to deliver their genetic cargo, far exceeding the 1% to 2% escape rate of other nanoparticle designs.
|
|
The findings, published in Science Advances (“Biodegradable targeted polymeric mRNA nanoparticles enable in vivo CD19 CAR T cell generation and lead to B cell depletion”), represent five years of collaborative work between biomedical engineer Jordan Green, Ph.D., the Herschel L. Seder Professor of Biomedical Engineering at the Johns Hopkins University School of Medicine, and immunologist Jonathan Schneck, M.D., Ph.D. The team merged Schneck’s expertise in artificial immune cells that stimulate other immune cells with Green’s polymer-based nanoparticle research.
|
|
The study advances the emerging field of in vivo immune cell engineering, which aims to reprogram a patient’s own immune cells inside the body rather than extracting and modifying them in a laboratory. CAR-T cell therapy, or chimeric antigen receptor T cell therapy, has proven effective against various blood cancers by removing a patient’s T cells, equipping them with cancer-detecting receptors, and reinfusing them. That process, however, remains expensive and time-consuming.
|
 |
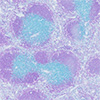
| Top image: Blue dyed B cells in the spleen of an untreated mouse. Bottom image: Reduction of blue B cells in the spleen of a mouse treated with the nanoparticles. (Image: Manav Jain and Jordan Green, Johns Hopkins Medicine) (click on image to enlarge)
|
|
“These experiments were successful using just one dose of the nanoparticles, and an advantage of using an off-the-shelf therapy is the potential for scalable manufacture and broad accessibility, whereas current forms of CAR-T therapies are very expensive and time-consuming,” says Green.
|
|
The nanoparticles are composed of polymers, strings of molecules called ester units that break down naturally in water. Their surface carries two antibody molecules, antiCD3 and antiCD28, which guide the particles to T cells and activate them. Inside, the nanoparticles carry mRNA, genetic instructions that direct T cells to produce surface receptors capable of identifying B cells associated with cancer and lupus.
|
|
Reaching T cells with nanoparticles presents particular difficulties compared with targeting localized sites such as the eye, Green explains. T cells naturally resist absorbing foreign particles, and even when particles get inside, the cells tend to degrade and expel them. “This makes sense, because if T cells easily internalize things like viruses, viral programming would take over the immune system, like what happens in HIV,” says Green.
|
|
The team developed a blend of antiCD3 and antiCD28 molecules that allows the nanoparticles to find and attach to T cells. Their testing showed that the biodegradable nanoparticles matched the performance of commercially available magnetic beads used in laboratory research for latching onto T cells, while also penetrating the cells to reprogram them from within. In a previous study, Green and his colleagues found that approximately 10% of their nanoparticles escape the cell’s degradation compartments to deliver their sensitive genetic cargo, compared with 1% to 2% for competing designs that are quickly broken down and ejected.
|
|
Green describes the nanoparticle mechanism as working in stages, comparing the process to how rockets travel to outer space, lifting off, engaging boosters, detaching them, and ultimately delivering their payload. In the current study, the nanoparticles degraded and released their mRNA contents within a few hours inside the mice.
|
|
After injection into healthy mice, 95% of the target B cells were depleted from circulating blood, and about 50% were destroyed in the spleen within 24 hours. One week later, B cells in the blood had returned to approximately 50% of their original levels.
|
|
Green, Schneck, and their Johns Hopkins colleagues have been named as collaborators with biotechnology company ImmunoVec on a more than $40 million grant from the Advanced Research Projects Agency for Health to develop these cell engineering tools. The research team plans to continue refining the nanoparticles, tailoring them more precisely to diseased B cells and adjusting the degree of T cell stimulation.
|
|
Other Johns Hopkins scientists who contributed to the research include Manav Jain, Savannah Est-Witte, Sydney Shannon, Sarah Neshat, Xinjie Yu, Sydney Dunham, Tina Tian, Leonardo Cheng, Jawaun Harris, Max Konig, and Stephany Tzeng. The research was supported by the Johns Hopkins Translational ImmunoEngineering Center, a National Center for Biomedical Imaging and Bioengineering focused on developing biotechnologies to modulate the immune system.
|
|
The polymer-based platform offers a potential path toward accessible, off-the-shelf immune cell therapies that bypass the individualized manufacturing process required by current CAR-T treatments. Whether these results translate from mice to humans remains to be determined, but the simplified three-component design and strong initial B cell depletion data position the approach as a candidate for further preclinical development.
|